A Silent Epidemic in Women’s Health
For millions of women across the world, painful periods, unexplained pelvic pressure, or difficulty conceiving are brushed off as “normal.” Yet behind these symptoms lies one of the most widespread but overlooked health conditions: Uterine Fibroids. By age 50, up to eight in ten women will develop fibroids—benign growths of the uterus that can silently undermine reproductive health, fertility, and quality of life.
Doctors often call Uterine Fibroids a “hidden threat” because they can grow undetected for years. In some cases, they remain harmless, but in others they cause debilitating pain, anemia, or repeated miscarriages. In Ghana and across Africa, where cultural stigma and limited resources make open discussions about menstruation rare, fibroids remain a shadow epidemic.
What Exactly Are Uterine Fibroids?
Uterine Fibroids, also known as leiomyomas or myomas, are non-cancerous tumors arising from the smooth muscle of the uterus. They vary in number, shape, and size—from tiny seed-like nodules invisible to the eye, to large masses that distort the womb and expand the abdomen.
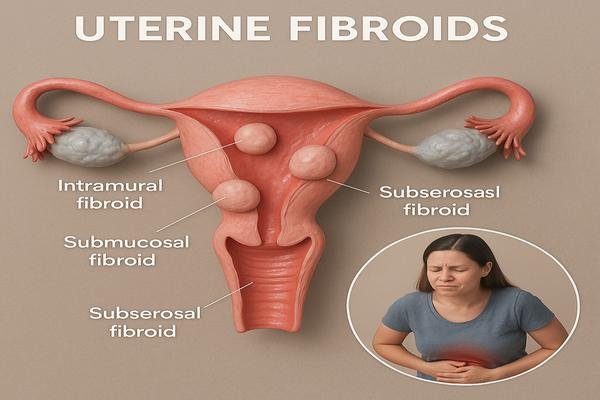
Specialists classify them into four types:
- Intramural fibroids: grow within the uterine wall
- Submucosal fibroids: grow under the inner lining and often affect fertility
- Subserosal fibroids: grow on the outer wall, pressing on nearby organs
- Pedunculated fibroids: hang by stalk-like attachments inside or outside the uterus
While not malignant, Uterine Fibroids can trigger heavy menstrual bleeding, pelvic pain, bloating, urinary problems, and miscarriages. Their silent growth means many women discover them only when they interfere with family planning.
Why Some Women Are More at Risk
Uterine Fibroids are not evenly distributed across populations. They disproportionately affect women of African descent. Studies show that Black women are nearly three times more likely to develop Uterine Fibroids, often at a younger age and with more severe symptoms.
Other risk factors include:
- Family history: If a mother or sister had fibroids, chances increase significantly.
- Obesity: Excess body fat raises estrogen levels, which stimulate fibroid growth.
- Early onset of menstruation: Girls who start periods before age 10 face higher lifetime risk.
- Hormonal exposure: Long-term use of estrogen-based contraceptives or therapy may elevate risk.
In Ghana, many gynecologists recommend routine screening for Fibroids in women over 25, especially those with a family history or heavy menstrual cycles. Early detection is key—delays often mean more invasive treatments later.
Signs Women Should Never Ignore
For some women, fibroids are silent passengers. For others, they wreak havoc on daily life. Warning signs include:
- Heavy or prolonged menstrual bleeding (menorrhagia)
- Periods lasting longer than seven days
- Pain during sexual intercourse
- Persistent pelvic pressure
- Frequent urination or constipation
- Swelling or enlargement of the lower abdomen
- Difficulty conceiving or recurrent pregnancy loss
Because these symptoms overlap with endometriosis or PCOS, many women go undiagnosed for years. Dr. Ama Konadu, an OB/GYN at Korle Bu Teaching Hospital, warns:
“Too many women live with Uterine Fibroids for years without knowing. Early detection expands treatment options and prevents devastating fertility problems.”
How Fibroids Are Diagnosed
Modern diagnostics have made detection easier, though accessibility remains an issue in many African health systems. Common tests include:
- Pelvic ultrasound – non-invasive and most widely used
- MRI scans – helpful in mapping multiple or large fibroids before surgery
- Hysterosonography – saline-infused ultrasound for cavity imaging
- Hysteroscopy – direct camera inspection of the uterine lining
- Lab tests – often to check for anemia caused by blood loss
The challenge is not technology but awareness and cost. Many women in Ghana delay testing because routine scans remain out of reach for low-income households.
Treatment Pathways: From Medication to Surgery
There is no one-size-fits-all treatment for Uterine Fibroids. Doctors weigh a woman’s symptoms, age, and fertility goals when recommending therapies.
Medical Options
- Hormonal therapy: birth control pills or IUDs to manage bleeding
- GnRH agonists: temporarily shrink fibroids by creating a menopause-like state
- Tranexamic acid: reduces menstrual blood loss
- Pain management: NSAIDs and supportive care
Surgical and Non-Invasive Procedures
- Myomectomy: surgical removal of fibroids while preserving the uterus
- Hysterectomy: complete removal of the uterus, ending fertility
- Uterine artery embolization (UAE): blocks blood supply, shrinking fibroids
- MRI-guided focused ultrasound (MRgFUS): non-invasive soundwave therapy
Fertility on the Line
Perhaps the most alarming impact of Fibroids is their effect on fertility. Submucosal fibroids are notorious for interfering with embryo implantation and causing miscarriages. Even intramural fibroids can distort the uterine cavity, complicating conception.
Encouragingly, treatment offers hope. Studies show that myomectomy can nearly double pregnancy rates. Fertility specialists also report higher IVF success after removing Uterine Fibroids.
Dr. Lydia Asare, a fertility specialist at Nyaho Clinic, explains:
“We’ve seen women conceive naturally after removing large Uterine Fibroids. It’s not a sentence—it’s a challenge that can be overcome.”
The African Burden
In Ghana and much of Africa, the crisis of Fibroids is intensified by stigma, financial barriers, and lack of education. Women often delay care because talking about menstrual pain is taboo.
Teaching hospitals offer surgeries, but costs remain prohibitive. Many women instead turn to herbal remedies or prayer camps, delaying medical treatment. NGOs such as UNFPA and Marie Stopes Ghana have stepped in with campaigns like “Know Your Uterus”, providing free screenings and community education.
Women Find Their Voices Online
Social media has opened new platforms for women to talk about Uterine Fibroids.
- Hashtags like #FibroidAwareness and #WombHealth trend across Instagram and TikTok.
- Ghanaian influencers candidly share their fibroid journeys.
- Health apps like Flo and Maya now include symptom trackers for fibroids.
Ama Owusu, a Ghanaian office worker, shared her story in a viral TikTok:
“I thought I was just unlucky with my periods—until I collapsed at work. Then doctors found Fibroids. Awareness saved my life.”
Global Health and Economic Challenge
Beyond personal suffering, Uterine Fibroids burden health systems and economies. In the United States, fibroid-related care costs billions annually. In Africa, untreated fibroids often mean infertility, mental health strain, and cultural stigma.
Public health experts argue that fibroid awareness should be elevated to the urgency of breast cancer and maternal mortality campaigns.
Breaking the Silence
Uterine Fibroids are not rare—they are an everyday reality for millions. With greater awareness, screening, and affordable treatment, this condition can shift from a silent epidemic to a managed challenge.
As Dr. Konadu stresses:
“Fibroids are common, but suffering in silence is not normal.”
Women everywhere deserve better awareness, earlier detection, and effective care to reclaim control over their reproductive health.